Prevalence of Salmonella spp., Listeria monocytogenes, Campylobacter spp. and Enterobacteriaceae in raw pet food

B. Boljkovac Begić*, K. N. Barać, M. Sablić, D. Mišetić Ostojić, K. Kvrgić and N. Džafić
Abstract
Raw feeding of dogs and cats is becoming increasingly popular worldwide. The raw material for such feed is muscles, offal and bones from mammals, fish or poultry. The production of such pet food is regulated by the European Commission legislation and should be carried out in a facility approved by the competent authority. Although proponents of such a diet point to the positive effects on the health and condition of the animals, studies have shown that raw pet food often contains pathogenic microorganisms. In the analysis of 28 samples of frozen raw pet food, we detected Salmonella spp. in 21.4% of the samples, Enterobacteriaceae more than 5000 cfu/g in 85.7% of the samples, Listeria monocytogenes more than 10 cfu/g in 39.3% of the samples, while Campylobacter spp.was below the limit of quantification in all samples. Of the eight samples containing poultry meat, Salmonella spp. was detected in five of them (62.5%), indicating that poultry is a high-risk raw material for Salmonella contamination.
Meanwhile, meat from domestic ungulates was identified as a high-risk source for Listeria monocytogenes, with that bacteria detected in 9 out of 20 (45%) of the samples containing this type of meat. The results indicate that hygiene in the production of raw pet food is unsatisfactory in most cases, that such food poses a risk to animal health and can be an indirect source of infection for humans via animal excretions and contaminated surfaces.Key words: raw pet food; BARF; Salmonella, Listeria, Campylobacter, Enterobacteriaceae
Introduction
Feeding dogs and cats raw food is increasingly popular worldwide (Michel et al., 2008; Wall, 2018). In example, Gregurin (2020) found that 22.73% of the search and rescue dogs of the Croatian Mountain Rescue Service were fed meals based on raw meat. In the Netherlands, 60.5% of owners feed their dogs raw meat in a certain percentage (Corbee et al., 2013), while in North America 25% of agility dogs are fed with raw meals (Dinallo et al., 2017).
Raw pet food can contain muscles, offal and bones of mammals, fish or poultry, as well as milk and eggs, and is prepared in the owner’s household or purchased as frozen food (Freeman et al., 2013). One of the concepts of feeding pets with raw food is BARF, initially an abbreviation for “bones and raw food”, and later the name “biologically appropriate raw food” became established (Billinghurst, 1993). Proponents of a raw meat diet point to the positive effects of such a diet on the immune system, the condition of the coat and skin, dental health, activity and general condition of the animals (Brozić et al., 2017).
In the European Union (EU), raw pet food may only be produced from category 3 material defined in Article 10 of Regulation (EC) no. 1069/2009, in a facility approved by the competent authority. The production should be controlled through a system based on the hazard analysis and critical control points (HACCP) principles (EC, 2009). According to Regulation (EC) 767/2009 (EC, 2009), the feed may only be placed on the market and used if it is safe and if it does not have a direct adverse effect on the environment or animal welfare.
The same Regulation lays down conditions for the labeling, packaging and presentation of feed, and mandates feed business operators to place on the market feed which is sound, genuine, unadulterated, fit for its purpose and of merchantable quality.
Commission Regulation (EU) 142/2011 requires the sampling of raw pet food to verify compliance with standards for Enterobacteriaceae and Salmonella as stated in Table 1 (EC, 2011).
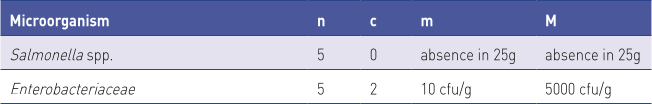
Where:
n – number of samples to be tested,
c – number of samples the bacterial count of which may be between m and M, the sample shall still be considered acceptable if the bacterial count of the other samples is m or less.
m – threshold value for the number of bacteria; the result shall be considered satisfactory if the number of bacteria in all samples does not exceed m;
M – maximum value for the number of bacteria; the result shall be considered unsatisfactory if the number of bacteria in one or more samples is M or more.
Human infections with Salmonella spp. are usually due to the consumption of contaminated food, but sometimes direct contact with animals, including dogs and cats, can also lead to infection (Hoelzer et al., 2011). For example, three cases of infection with multidrug- resistant Salmonella ser. Typhimurium have been reported in employees and clients of veterinary organizations and animal shelters.
The cases involved a total of 20 people and several cats, and although it is not known how the human patients in these outbreaks became infected with Salmonella, the authors hypothesize that accidental ingestion of animal feces could cause human infection (CDC, 2001).
There has also been one case of monophasic Salmonella ser. Typhimurium in two children and three dogs in same household. Again, the route of transmission was not determined, but the authors proposed several transmission hypotheses, one of which was transmission of Salmonella from dogs to children (Russini et al., 2022). Studies have shown that dogs fed raw food are 30 times more likely to excrete Salmonella spp. than those fed dry food (Joffe and Schlesinger, 2002; Viegas et al., 2020) and that excretion can last up to 14 days after consumption, while infections are mostly asymptomatic (Finley et al., 2007).
Infection of poultry with Campylobacter is common and in humans campylobacteriosis causes enteritis. Various Campylobacter species are also frequently isolated from dogs (Bojanić et al., 2019). In examinations of dog feces, Campylobacter were isolated in 26.3% to 36.4% of samples, and it was significantly more often detected in dogs with diarrhea and young dogs (Vidović Popek, 2014; Štritof et al., 2018; Švob, 2018).
Listeria monocytogenes is ubiquitous and has been isolated from 60 species of animals, including 29 mammalian and 24 avian species (WOAH, 2021), one of which are gulls (Humski et al., 2022). This bacterium causes abortions and perinatal mortality, and ruminants serve as an important reservoir for this microorganism and play a central role in its transmission from animals to humans.
They can be asymptomatic carriers or develop encephalitis or meningoencephalitis and Listeria keratoconjunctivitis and uveitis (“silage eye”), fetal infections and, on rare occasions, mastitis (Končurat and Sukalić, 2024; Boljkovac Begić et al., 2025). Monogastric animals mainly develop septicemia, while in healthy humans listeriosis manifests as fever and limited gastroenteritis. Children, the elderly and immunocompromised patients are susceptible to listeriosis in whom it causes meningitis, encephalitis, altered mental status and sepsis, while pregnant women are at risk of abortion.
While listeriosis is uncommon in humans, it is associated with frequent hospitalizations, and has a high mortality rate. In 2017, over 2,400 cases were reported across EU countries (Končurat and Sukalić, 2024).
The fact that Salmonella can remain on the pet food bowls even after washing and cleaning (Weese and Rousseau, 2006) and that Campylobacter spp., Listeria monocytogenes and Salmonella spp. can form a biofilm (Stepanović et al., 2004; Janež et al., 2021; Klančnik, et al., 2021; Shatila et al., 2021) makes contaminated pet food a potential source of infection for animals and humans (El-Liethy et al., 2020).
The aim of this study was to determine the presence of Salmonella spp. and the number of Enterobacteriaceae, Campylobacter spp. and Listeria monocytogenes in raw pet food marketed in the Republic of Croatia.
Material and methods
Samples of raw pet food (n=28) were collected from a retail store for research purposes. All samples were delivered frozen in packages of 250 to 500 g. They were brought to the laboratory within 30 minutes in portable cool boxes and stored at < -20°C until analysis. The samples came from three producers and from different types of meat: beef (12 samples), beef and fish (4 samples), chicken (4 samples), one sample each of game, rabbit, lamb, horse, duck, veal with chicken, chicken with turkey and lamb with chicken.
Depending on its origin, the raw material was divided into three groups: meat from domestic ungulates (U), poultry (P) and meat from other species than domestic ungulates and poultry (O). On this basis, the samples ware grouped as shown in Table 2.
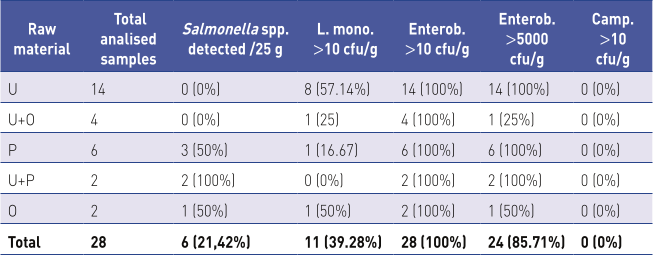
U – meat from domestic ungulates
P – meat from poultry
O – meat from other speices than domestic ungulates and poultry
U+O – combination of meat from domestic ungulates and meat from other speices than domestic ungulates and poultry
U+P – combination of meat from domestic ungulates and meat from poultry
L. mono – Listeria monocytogenes
Enterob. – Enterobacteariaceae
Camp. – Campylobacter spp.
To determine the presence of Salmonella spp. the method according to ISO 6579-1:2017 was applied, using XLD agar ISO formulation (Biolife Italiana S.r.l, Italy) and Chromogenic Salmonella Agar (Biolife Italiana S.r.l, Italy) for plating. Taylor Lysine Decarboxylase Broth, Urea agar prepared according to Christensen and Triple Sugar Iron Agar ISO (Biolife Italiana S.r.l, Italy) were used to determine the biochemical characteristics of the prusumptive Salmonella spp., while polivalent and monovalent Salmonella antisera (Bio-Rad Laboratories, Inc., USA) were used for serological group identification.
Listeria monocytogenes was counted according to ISO 11290-2:2017 by inoculation of 1 ml of initial suspension and decimal dilutions on the surface of ALOA (Biolife Italiana S.r.l, Italy) in a 140 mm Petri dish, and confirmation was done by further testing of the suspected colonies. Blood agar plates prepared from Blood Agar Base (Biolife Italiana S.r.l, Italy) with sheep blood additive (BIOSAP SO, Biognost d.o.o., Croatia) were inoculated and incubated at 37+/-1°C for 24 +/-2 hours to examine hemolysis. API Listeria (bioMérieux SA, France) was used for the utilization of L-rhamnose and D-xylose and for other tests.
Enterobacteriaceae were enumerated according to ISO 21528-2:2017, while the number of Campylobacter spp. was determined by inoculating 1 ml of the initial suspension and further decimal dilutions onto three plates of Campylobacter Blood-Free Selective Agar (Oxoid Ltd, United Kingdom) with a diameter of 90 mm and incubating for 44+/-2 hours at 41.5+/-1°C under microaerophilic conditions.
Results
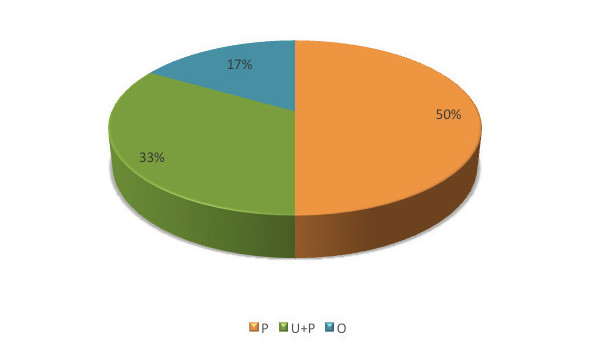
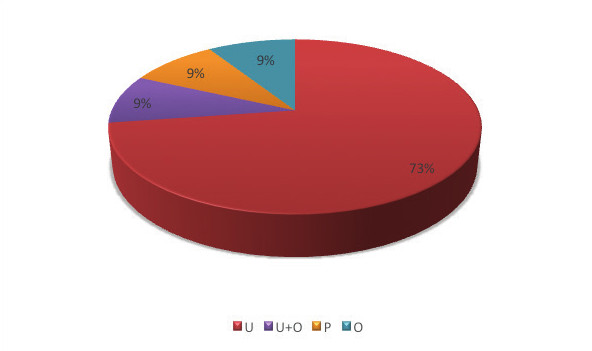
Of the 28 samples analyzed, Salmonella spp. were isolated from six samples (21.4%), five of which belonged to serological group O:7 and one to group O:4. Of the six samples in which Salmonella bacteria were detected, five contained poultry meat (83.33%). Enterobacteariaceae were found in all 28 samples, with the number of colony-forming units per gram (cfu/g) exceeding 5000 in 24 samples (85.7%). The number of Campylobacter spp. was below the limit of quantification in all samples, while Listeria monocytogenes was counted in 11 samples (39.3%), with the count exceeding 100 cfu/g in two samples. Of the 11 samples in which Listeria monocytogenes was found, 9 of them contained meat from domestic ungulates (81.8%). The results are shown in Table 2 and Figures 1, 2, 3 and 4.
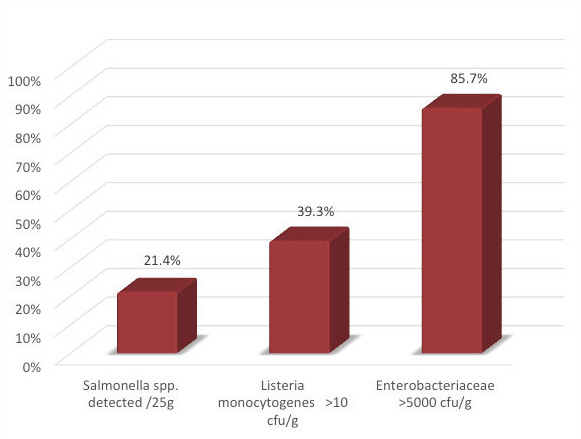
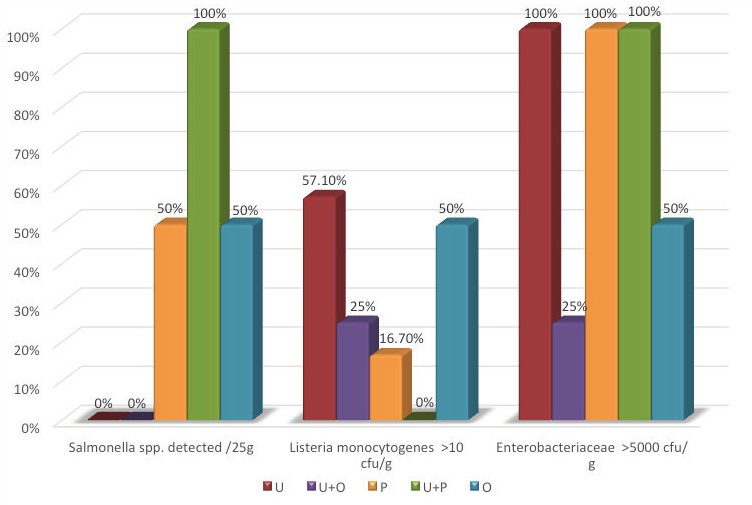
Discussion
For raw pet food, Commission Regulation (EU) 142/2011 stipulates that Salmonella may not be present in 25 g and that the number of Enterobacteriaceae may not exceed 5000 cfu/g in any of the five sample units and that no more than two out of five units may have an Enterobacteriaceae count between 10 cfu/g and 5000 cfu/g. None of the samples tested contained less than 10 cfu Enterobacteriaceae per gram. In four samples the number of Enterobacteriaceae was determined between 10 cfu/g and 5000 cfu/g and for these it is not possible to determine the conformity, as no data are available for the other four sample units. In 24 out of 28 samples, the number of Enterobacteriaceae was determined to be more than 5000 cfu/g, which means that 85.7% of the samples do not comply with the provisions of Commission Regulation (EU) 142/2011.
Of the 28 samples tested, Salmonella spp. were found in six samples, which means that 21.4% of the samples are unsafe for human and animal health. Infections of dogs with bacteria of the genus Salmonella are usually asymptomatic (Finley et al., 2007), but clinical cases of disease have been described in dogs fed raw food, such as one case of septicemia and thrombocytopenia (Albuquerque et al., 2021) and two cases of septic peritonitis caused by resistant bacteria of the genus Salmonella (Binagia and Levy, 2020). In cats fed raw food, there have been cases of clinical salmonellosis in a form of septicemia and gastroenteritis (Stiver et al., 2003), and lower urinary tract disease and bacteriuria (Fauth et al., 2015). Although only 0.1% of pet owners believe they have become infected through handling pet food (Anturaniemi et al., 2019), the possibility of infection cannot be ignored.
Such was a case where 70 human infections with the species Salmonella enterica ser. Schwarzengrund were reported in the United States in 19 states caused by contaminated pet food (CDC, 2008). A significant increase in the number of human infections with Salmonella ser. Infantis was also described in Canada in 1999, which was associated with contaminated pig ears – pet treats (Clark et al., 2001).
Of the six samples in which the presence of Salmonella spp. was detected, five samples contained poultry meat (83%), and of the total eight samples containing poultry meat, Salmonella spp. was detected in five samples (62.5%), indicating that poultry is not a safe raw material for the production of raw pet food.
The number of Campylobacter spp. was below the limit of quantification in all samples, which may be a consequence of the sensitivity of the bacterium to freezing (Georgsson et al., 2006; El-Shibiny et al., 2009).
Listeria monocytogenes was enumerated in 11 samples (39.3%), with two samples exceeding 100 cfu/g. Of the 11 samples in which Listeria monocytogenes was found, 9 contained meat from domestic ungulates (81.8%), and of the total of 20 samples containing meat from ungulates, that bacteria was counted in 9 (45%). Notably, 95% of the ungulate meat was from ruminants, which Končurat and Sukalić (2024) identified as a known reservoir for Listeria. Our findings therefore align with their research and indicate that meat from domestic ungulates is high risk raw material with regard to Listeria monocytogenes.
The manufacturers of raw pet food recommend thawing the products in the refrigerator, at room temperature or in lukewarm water before use and point out that an opened and thawed product can be stored in the refrigerator for up to 24 hours. Since Listeria monocytogenes is able to multiply even at refrigerator temperature (Boljkovac, 2012; Myintzaw et al., 2023), this recommended procedure creates conditions for the multiplication of these bacteria in the product and on other objects and surfaces with which contaminated pet food can come into contact. The presence of Listeria monocytogenes above 10 cfu/g in 39.3% of samples in combination with the procedure recommended by the manufacturers, makes raw pet food a risk to human and animal health. In humans, listeriosis manifests itself in three clinical syndromes: maternofetal listeriosis or neonatal listeriosis, bloodstream infection and meningoencephalitis. As a result of hematogenous spread, focal infections can occur, most commonly in the peritoneum, joints, endocardium or eyes (Swaminathan and Gerner-Smidt, 2007). Listeriosis affects the elderly, children, immunocompromised individuals and pregnant women, while it causes fever and gastroenteritis in healthy people (Končurat and Sukalić, 2024).
Listeriosis in dogs and cats is not common, but there are various forms and routes of infection. For example, a case of abortion has been reported in a bitch that became infected after being fed contaminated raw meat (Weber and Plagemann, 1991), as well as cases of septicemia (Pritchard et al., 2016), myocarditis (Wong and Hugo, 2021), osteomyelitis (Genain et al., 2017), cutaneous listeriosis (Loncarevic et al., 1999), as well as a case of generalized listeriosis leading to the death of a dog (Schroeder and van Rensburg, 1993), and other forms (Läikkö et al., 2004; Marien et al., 2007; Palerme et al., 2016; Musser et al., 2019).
The results obtained are comparable with those of other studies. In a study conducted in Sweden, for example, 52% of the samples did not meet the EU’s hygiene requirements for the production process, Salmonella species were isolated from 7% of the samples and Campylobacter species from three samples (Hellgren et al., 2019). In another study, Salmonella was isolated from 15 and Listeria monocytogenes from 32 samples out of a total of 196 samples of raw pet food (7.7% and 16.3%). In contrast, out of 480 samples of dry and semi-moist pet food Salmonella species were isolated from one sample and Listeria monocytogenes from none (Nemser et al., 2014). In Japan, 12% of samples of raw pet food were contaminated with Salmonella (Yukawa et al., 2022) while in Italy Salmonella species were isolated from 71 % of the analysed samples. In the same study, the bacterium Listeria monocytogenes was isolated from 90% and Campylobacter from 29% of the samples examined (Bottari et al, 2020). A higher percentage of positive samples than in our study is probably due to the different methods used.
These pathogens are zoonotic, and often originate from farm animals used in raw pet food production. Pets consuming contaminated raw diets can become asymptomatic carriers, shedding these pathogens in their feces and potentially contaminating environment. Therefore, a One Health approach is necessary to prevent the further spread of bactera and protection of human and animal health (Ferri, 2023).
Conclusion
It can be concluded from the results that hygiene in the production of raw food is not satisfactory in most establishments, as shown by the increased number of Enterobacteriaceae in 85.7% of the samples.
The pathogenic microorganism Listeria monocytogenes was isolated in 39.3% of the samples and Salmonella spp. in 21.4% of the samples, which is why raw pet food pos es a risk to animal and human health.
Significantly, Salmonella spp. was detected in 62.5% of samples containing poultry, making poultry meat a high-risk raw material for raw pet food. Manufacturers should use poultry meat that is free from Sallmonella spp., as determined by legislation.
Listeria monocytogenes was detected in 45% of samples containing meat from domestic ungulates. Additionally, meat from domestic ungulates accounted for 81.8% of Listeria– positive samples, suggesting that meat from domestic ungulates is a high-risk raw material for Listeria monocytogenes contamination.
Pet owners must be made aware that raw pet food, feeding bowls, the refrigerator and all surfaces with which raw pet food comes into contact, as well as the bodies and feces of animals, can be a source of infection.
Therefore, increased hygiene and disinfection of surfaces, dishes and feeding bowls with which raw pet food comes into contact is necessary, especially if pregnant women, children, elderly or immunocompromised people live in the household.
References [… show]
Određivanje pojavnosti Salmonella spp., Listeria monocytogenes, Campylobacter spp. i Enterobacteriaceae u sirovoj hrani za kućne ljubimce
Barbara BOLJKOVAC BEGIĆ, dr. med. vet., viša stručna suradnica u sustavu znanosti; Karmela Nina BARAĆ, dr. med. vet., stručna suradnica u sustavu znanosti; Mirela SABLIĆ, dr. med. vet., stručna suradnica u sustavu znanosti; Dijana MIŠETIĆ OSTOJIĆ, prof., viša stručna suradnica u sustavu znanosti; dr. sc. Kristina KVRGIĆ, viša stručna suradnica u sustavu znanosti, dr.sc. Natalija DŽAFIĆ, znanstvena suradnica, Hrvatski veterinarski institut – podružnica Veterinarski zavod Rijeka, Hrvatska
Hranidba pasa i mačaka sirovom hranom sve je popularnija u svijetu. Sirovina za njenu proizvodnju su mišići, organi i kosti sisavaca, ribe ili peradi.
Proizvodnja takve hrane za kućne ljubimce regulirana je zakonodavstvom Europske komisije i treba se provoditi u objektu koji je odobrilo nadležno tijelo. Iako zagovornici takve prehrane ističu pozitivne učinke na zdravlje i opće stanje životinja, istraživanja su pokazala da sirova hrana za kućne ljubimce često sadrži patogene mikroorganizme. U analizi 28 uzoraka smrznute sirove hrane za kućne ljubimce detektirali smo Salmonella spp. u 21,4 % uzoraka, Enterobacteriaceae u broju većem od 5000 cfu/g u 85,7 % uzoraka, bakteriju Listeria monocytogenes u broju većem od 10 cfu/g u 39,3 % uzorka, dok je broj Campylobacter spp. bio ispod granice kvantifikacije u svim uzorcima. Od osam uzoraka koji su sadržavali meso peradi, Salmonella spp. je detektirana u pet (62,5 %), što ukazuje da je perad sirovina visokog rizika za kontaminaciju Salmonellom. Meso domaćih papkara i kopitara prepoznato je kao visokorizičan izvor za Listeria monocytogenes, jer je ta bakterija otrkivena u 9 od 20 (45 %) uzoraka koji su sadržavali ovu vrstu mesa. Rezultati ukazuju da je higijena u proizvodnji sirove hrane za kućne ljubimce u većini slučajeva nezadovoljavajuća. Takva hrana predstavlja rizik za zdravlje životinja i može biti neizravan izvor zaraze za ljude putem životinjskih izlučevina i kontaminiranih površina.Ključne riječi: sirova hrana za kućne ljubimce, BARF, Salmonella, Listeria, Campylobacter, Enterobacteriaceae

